March 25, 2026
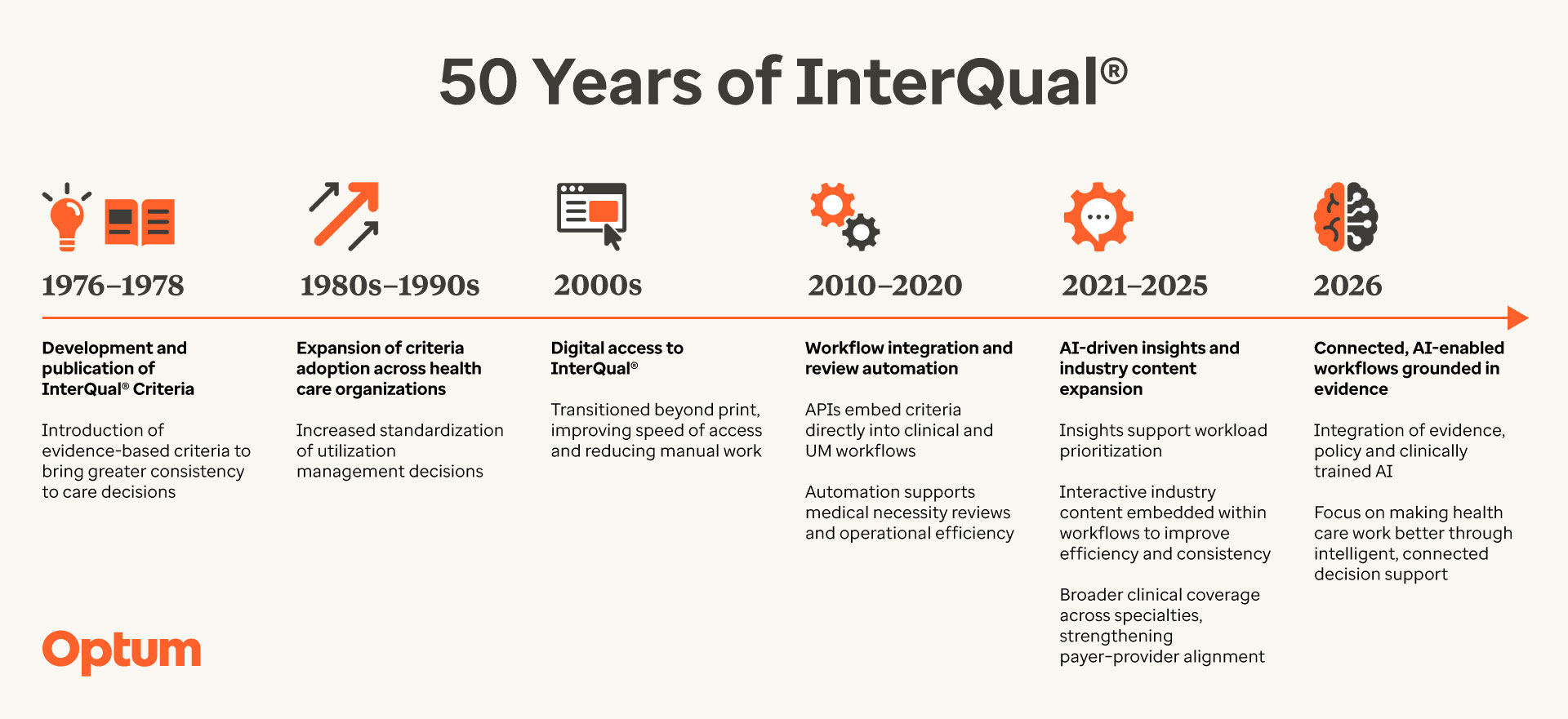
InterQual 2026 marks 50 years of clinical rigor, advancing automated, evidence-based care
March 24, 2026 — For 50 years, InterQual® has provided a trusted, evidence-based approach to decision support. That legacy reflects Optum’s broader commitment to creating solutions that simplify health care, especially as regulatory requirements evolve and administrative demands increase. Today, hospitals and health plans face mounting complexity that can delay decisions and risk patient access to appropriate care.
InterQual 2026 builds on the five-decade foundation by combining up-to-date content with AI-enabled automation to simplify utilization management (UM) review processes, make decisions easier to explain, and help information flow more smoothly across the care journey.
“InterQual criteria has always been grounded in objective, evidence-based medicine,” said Laura Coughlin, vice president of clinical innovation and development at Optum Insight. “The 2026 release integrates complex policy guidance directly into daily workflows and advances responsible AI and automation that support clearer, more consistent decisions for patients.”
Embedded policy guidance at the point of review
Growing volume and complexity in UM require tools that help reduce the manual effort for review teams. InterQual 2026 supports compliant, accurate decisions by applying policy and evidence-based standards directly within the workflow, so reviewers spend less time searching for information and more time moving decisions forward. These updates include:
- Medicaid Policy Navigator delivers FHIR based, interactive policy guidance embedded to help support compliance and faster reviews. Medicaid is a critically complex environment, where policies vary across all 50 states and multiple sources, increasing manual effort, and complicating medical necessity decisions as requirements change.
- LOCUS Navigator offers access to the Level of Care Utilization System (LOCUS) assessment within the UM workflow application through a partnership with the American Association for Community Psychiatry and Deerfield Solutions LLC, helping teams make consistent level-of-care decisions across mental health and addiction settings.
Clear communication builds trust
In today’s fragmented health care system, transparent communication is essential to building trust and keeping care moving forward. The Decision Reasons module delivers clear, plain-language explanations to help patients and providers understand why a service may not be clinically appropriate. This year’s expanded library now supports rationale content for imaging and Medicare-related determinations, along with new provider summaries to streamline communication, reduce manual work, and improve consistency.
“Decision Reasons has transformed how we communicate medical necessity decisions by improving efficiency, consistency, and audit performance while eliminating the need to manage our own library of explanation content,” said Julie Schmitz, RN, BS, director of utilization management at Kelsey Seybold Clinic. “Clear, empathetic explanations reduce confusion for patients and providers, and have saved our team significant time.”
Regulatory ready connectivity and responsible automation for better access
Health plans and clinicians are under growing pressure to make timely, well supported care decisions. At the same time, intensifying regulatory oversight is driving UM to meet higher standards for timeliness and connectivity, including those mandated by CMS 0057. InterQual 2026 is designed to support these expectations by reducing delays and preserving clinician led decision making through advancements such as:
- Digitized, interoperable content delivered through InterQual Exchange, which provides InterQual Criteria, industry content, and custom policies via FHIR-based APIs.
- Expanded automation with InterQual AutoReview, now supporting 98% of condition-specific, day-one reviews and 58% of continued-stay reviews to help reduce administrative work, improve consistency, and expedite medical necessity decisions.
- InterQual® Auth Accelerator, announced earlier this year, uses AI to evaluate provider-submitted documentation against relevant InterQual Criteria, supporting faster, accurate prior authorization review. The AI model is developed and continually refined by the same clinical experts who create the criteria, helping maintain clinical integrity, and ensuring care decisions remain firmly in human hands.
Advancing clarity and connection across care
As a leader in UM, Optum is reshaping how decision support is delivered by making it more connected, easier to use, and better aligned to continuity of care. This work is part of a broader commitment to make the health system simpler and more supportive for the people and communities served by reducing avoidable delays and improving clarity at every step. The goal is simple: a clearer, faster, more consistent care experience that improves the patient journey — even if they never see the technology behind it.